Atrial fibrillation
Atrial fibrillation is a condition in which the heart beats irregularly due to chaotic electrical signals that come from the upper chambers (atria) of the heart.
upbeat.org/heart-rhythm-disorders/atrial-fibrillation
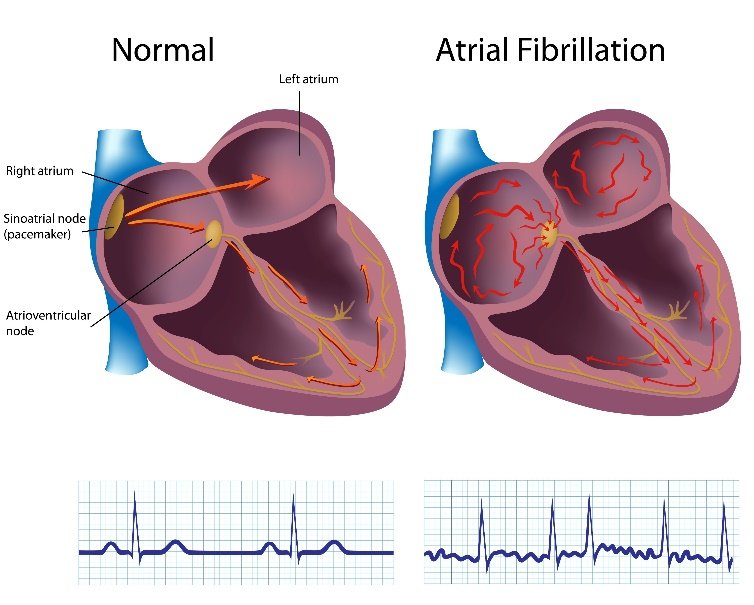
How is atrial fibrillation diagnosed?
If you are suspected of having atrial fibrillation, your doctor may perform an electrocardiogram (also known as an ECG). This involves putting small dots across the chest that are connected to leads which measure the electrical activity of the heart and can detect atrial fibrillation.
You may have to wear a portable version of these leads for 24hrs to detect shorter episodes of atrial fibrillation or other abnormal rhythms. This is called a Holter monitor.
Blood tests can be performed to look for triggers of AF such as an overactive thyroid. Sometimes sleep studies and lung function tests are performed if it is suspected that sleep apnoea or lung disease is present.
Other tests include an echocardiogram, which is an ultrasound of the heart to look for heart failure or valve problems.
What causes atrial fibrillation?
There is no single cause of atrial fibrillation. However, there are many conditions that it is associated with:
- increasing age
- other heart conditions such as coronary artery disease, heart failure and heart disease related to high blood pressure
- other medical condition including overactive thyroid or hyperthyroidism, obstructive sleep apnoea, chronic kidney disease, diabetes and chronic lung disease
- lifestyle factors including obesity, smoking, alcohol and binge drinking
Why does detecting atrial fibrillation matter?
Atrial fibrillation can cause two major issues:
- symptoms – due to an inadequately controlled heart rate, often causing palpitations or racing heart beat, breathlessness on exertion or chest pain. Some patients may have minimal or no symptoms.
- an increased risk of stroke (even in the absence of any symptoms) – this risk depends on your age and other medical issues
To understand more about the symptoms and effects of stroke, connect to the Stroke Foundation website below for some excellent videos:
strokefoundation.org.au
What treatments are available for atrial fibrillation?
For symptoms/rhythm management:
- medication can be trialled to decrease the amount of time you spend in atrial fibrillation or to control how fast your heart pumps when in AF
- an electrical cardioversion may be recommended
- if a specialised procedure called as a catheter ablation for AF might be helpful, you will be referred on to a specialist with particular expertise in this area.
For more information on catheter ablation, see the link below:
upbeat.org/common-treatments/catheter-ablation
Assessing and decreasing stroke risk
If your risk of stroke is deemed to be high, your doctor may also recommend blood thinners to be taken every day. This can help in reducing your risk of stroke.
Lifestyle
Even when you have already had one or more episodes of atrial fibrillation, leading a healthy lifestyle can help to prevent a further episode. This includes having a healthy diet, regular exercise and abstaining from smoking and drinking.

